ARTICLE
Safety of biomaterials, particularly allogenic and xenogeneic materials, has always been an important topic. In current times, some clinicians and patients are more anxious and increasingly interested in material safety. This is an essay about the safety of biomaterials during corona times also in the view of the new Medical Device Regulation (MDR).
Patient information in the times of COVID-19
The role of patient information has not changed in these challenging times, however the requirements of patient communication before surgery have increased. Many patients are unsettled by the media and are afraid of the risk of infection. This can cause them to postpone treatments that are supposedly unnecessary to avoid going to the doctor or dentist, which can then lead to devastating consequences for their health.
Doctors and dentists who are currently prospering have understood how to gain the trust of patients. They have adapted their practice procedures and hygiene concepts so that patients feel safe already before their surgical procedure. Dental providers need to implement initiatives to support practices during these difficult times. By means of a thorough patient education, clinicians should continue to discuss the origin and possible risks of animal, synthetic or human-derived products, as was done before.

Changes in risk analysis for biomaterials in view of the new MDR and COVID-19
For allogenic tissue preparations, for example maxgraft®, nothing will change once MDR has come into full force: tissue preparations, unlike derivatives will remain within the scope of Directive 2004/23/EC, which regulates the donation, procurement and testing of human tissue throughout Europe. For example in Germany, this means that human tissue products sourced from tendon, cartilage, bone and skin, will continue to require a pharmaceutical level of approval and will not fall under the Medical Devices Act. In other countries for example in the UK, those tissue preparations will continue to be regulated as human tissues and not medical devices. A comprehensive statement on this issue with the corresponding sources can be requested from botiss.

An important change with the introduction of MDR will be stricter post-market clinical surveillance of medical devices, as well as stricter requirements for the provision of clinical evidence of Class III medical devices. This means that the powers of the Notified Bodies will increase and that in the future there will be more unannounced audits, random tests and product tests. There will also be even stricter requirements for product safety and performance. As a result, manufacturers will increasingly be obliged to document clinical data.
For established products, hardly anything will change provided that:
- the products have been on the market for a long time
- sufficient clinical data are available in the form of studies/publications
- a good post-market surveillance system has been put in place
botiss is therefore well positioned to meet the increased requirements, even after the introduction of MDR.
All implantable materials of animal origin and materials that are degraded to a considerable extent in the body, such as synthetic bone grafting materials and collagen membranes were already classified as Class III medical devices under the previous Medical Device Directive. This means that these products were already subjected to very high regulatory requirements and safety standards. For example, all products originating from an animal must annually be monitored for zoonosis. The monitoring needs to account for diseases that can be transmitted from animals to humans which are known or are emerging. In addition, zoonosis monitoring evaluates and assesses the measures that have been taken to reduce or eliminate the risk of transmission (e.g. hygiene rules in the retrieval of raw materials or specific steps during the production process to inactivate pathogens). A transmission of potential SARS-CoV-2 viruses can be excluded due to these established measures for virus inactivation.
Both the high temperature treatment of xenogeneic materials (such as cerabone®) and chemical treatments using ethanol and hydrogen peroxide, as performed for allogenic bone grafts and collagen-based products from botiss, effectively inactivate viruses including the SARS-CoV-2 virus (1). Details of the chemical treatment for allograft processing are given below.
Preparation and characteristics of allogenic materials
The main advantage of allografts is the ability to transfer from human donor to recipient a bone graft that has a biologically valuable composition and structure. This enables genuine remodeling to take place as allografts can be resorbed and replaced by vital bone. This was impressively demonstrated by histological examinations after the use of maxgraft® cancellous bone granules (2).
It is common practice to perform a heat treatment on xenogeneic bone grafting materials, yet this approach is not valid for allografts. Thermal treatment of human tissue would degrade the allogenic bone grafts, reducing their biological potential and drastically reduce their resorption rate to give characteristics similar to that of xenogeneic bone grafts, yet with a significantly reduced availability and considerably higher costs. Therefore, chemical treatments are performed instead to preserve more of the allograft’s biologically important components.
botiss allografts contain bone tissue from cancellous, cortico-cancellous, or cortical bone. In contrast to products produced from the so-called derivatives of human or animal tissue, in which individual substances are isolated from the tissues, the structure and composition of the allografts are retained, but with the almost complete removal of all cellular substances.

Contrary to the misassumption that all organic components of allografts must be removed by the preparation process, those components are precisely what should be retained. As in native bone, the organic components make up approximately 30 percent of the bone structure, which is mainly collagen. In comparison, almost every collagen membrane is composed of 100 percent animal organic components and is nevertheless used at any time and quite rightly without hesitation. If the collagen were to be completely removed from the allogenic blocks, it would create a pure anorganic but very brittle block, which could be difficult to fix with a screw.
Alternatively, it is possible to mix a pure mineral bone grafting material with collagen, e.g. of porcine origin, and produce a so-called composite material. There are some materials on the market that follow this approach. These materials can indeed – compared to purely mineral products – have improved biological properties due to the collagen they contain. However, they generally have a mechanical and resorption stability inferior to that of allogenic blocks, which makes them rather unsuitable for block augmentation.
Safety of allografts
To guarantee the safety of the allogenic biomaterials, a whole range of measures are prescribed by law. These include in the case of the botiss maxgraft® product line (AlloTec® process by C+TBA)
- the donor medical history
- serological tests using antibody screening and PCR (polymerase chain reaction)
- continuous microbiological testing
- a complex wet-chemical disinfection and degreasing
- gamma irradiation of the packaged units
Regarding special corona measures in place at the tissue banks, potential risks associated with the handling of materials of human origin are, in any case, continuously monitored and the processes adapted accordingly, if necessary. Tissue banks are therefore well prepared and the corona pandemic is anything but critical with regard to the safety concept for the supply of products of human origin.

The processing of human tissue offers the necessary safety for preventing the transmission of SARS-CoV-2 viruses. The staff at the botiss partner tissue bank Cells and Tissue Bank Austria (C+TBA), based in Krems, Austria have always worked under extremely high hygienic conditions in a clean room when handling the donated tissue. To protect the staff, no corona-specific precautions beyond the normal level are necessary during the pandemic and beyond.
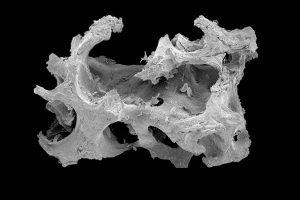
The C+TBA has carried out a corresponding risk analysis early on after the discovery of SARS-CoV-2. This showed that individual steps of the established chemical process already effectively eliminate potential SARS-CoV-2 viruses (3). The treatment with three percent hydrogen peroxide and ethanol in various concentrations penetrates deep into the tissue and is a recognized standard for disinfection after potential contamination with SARS-CoV-2 (1). The processes are designed to effectively inactivate a wide range of different potential pathogens (fungi, spores, bacteria, RNA and DNA viruses – both enveloped and non-enveloped – with different resistances). In this way, even newly discovered or yet unknown pathogens can be covered by the process with a high degree of probability.
Furthermore, dry storage over weeks to months until the finished processed tissue is used offers a draining effect, as the virus only has an infectivity of a few days on various surfaces (4). Nevertheless, one should not forget that the main transmission route is a droplet or smear infection. The highest viral load is found in the respiratory tract and the viral load in serum, for example, is already significantly lower than in sputum (5). The virus load in the bone of infected persons is low, if existing at all. Therefore, speculations about infections during bone augmentation procedures are rather hypothetical. Transmission through blood or tissue has not been described so far and as long as the tissue preparations undergo a validated virus inactivation procedure no additional measures such as SARS-CoV-2 testing of the donors or evaluation of the travel history are necessary according to the German authority Paul-Ehrlich-Institute.
Xenogeneic materials as an alternative
The safety of cerabone® is based on a different principle, the high temperature treatment during the manufacturing process. In the production of the bovine grafting material, the raw material is gradually heated to over 1200°C using a sophisticated process. Apart from the temperature, only water is used for rinsing, so the processing is free of chemical additives.
The heating process safely removes all organic components such as cells and proteins, as well as bacteria and viruses. The process even inactivates prions, which are the cause of Variant Creutzfeldt Jakob disease (6). At the same time, a high degree of crystallinity (7) is achieved by this manufacturing process. Both factors contribute to cerabone®’s exceptional volume stability and ensure that it remains permanently in the augmented area after implantation. Unlike with allogenic material, there is no remodeling, which is desirable for certain indications. These include the augmentation of horizontal defects in the esthetic area, resorption protection for augmentations using autologous or allogenic bone blocks, and socket preservation, particularly if it is not yet clear whether an implant is to be placed and when.

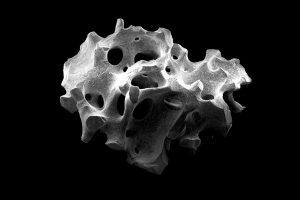
Unlike occasionally stated, high-temperature treatment does not generally have a negative influence on the graft surface and porous structure. This is dependent on the respective production process. cerabone®, due to the slow and sustained heating of the bone raw material, has a very good osteoconductivity and hydrophilicity (8, 9). Because of the increasing interest in the topic of high temperature treatment, botiss has created the homepage 1200trust.com. It contains all information about the unique production process of cerabone® and its influence on the safety and properties of the product, as well as many examples (clinical cases, videos, webinars) of its clinical application.
Synthetic materials as an alternative without human or animal origin
Despite the high safety of allogenic and xenogeneic grafting materials due to their specific manufacturing processes, some people are afraid of using these types of materials. For these clinicians or patients, synthetic materials can provide an alternative. Synthetic bone substitute materials, mostly based on calcium phosphate, have been available in the dental sector for a long time. In recent years however, confidence in synthetic products has not been as high as for bovine bone. This is perhaps due to the inhomogeneity between synthetic biomaterials. The available synthetic biomaterials comprise of a large number of very different materials with correspondingly very different properties. In the dental sector, biphasic materials made of hydroxyapatite and beta-tricalcium phosphate have become particularly popular, such as maxresorb® from botiss. Due to their composition of a rapid and a slow resorbing component, they offer controlled resorption and have shown that they are a valid alternative to human or bovine products in a variety of indications. At present, there can be seen an increasing trend towards synthetic materials on the market.


With regards to synthetic barrier membranes, in 2017 botiss launched the blue membrane permamem® as an alternative to xenogeneic membranes. Since then, the non-resorbable high-density PTFE membrane has become very popular with dentists because it is very thin and therefore extremely easy to handle. Apart from its synthetic origin, permamem® also offers other advantages over collagen membranes. Since it is not resorbed and as its highly dense structure prevents the penetration of bacteria, the permamem® membrane can also be used for open wound healing in certain indications such as socket or ridge preservation (10). In addition, it has a higher dimensional stability than collagen membranes and is therefore also suitable for augmentations outside the ridge contour.
The share of synthetic materials in the regenerative field will certainly grow in the coming years. The trend cannot be ignored, if one thinks about the many vegan products that are currently on the market. This trend is happening in a lot of industries, from cosmetics to fashion to the food industry. Whereas ten years ago, a vegan restaurant was still an exotic thing, nowadays it is impossible to imagine European cities without them. The topic “vegan lifestyle” has reached the mainstream of society. But there are some markets on the global scale that prefer synthetic materials for other reasons, e.g. religious beliefs.
As a full-service provider in the field of biomaterials, botiss has the claim to offer premium products for all areas of regeneration. The individual patient and his or her specific needs are the focus of attention. Every patient and every case have individual requirements. In order to achieve optimal and predictable results, the products may have to be combined – this may be to meet the requirements of certain indications. This is the reason why our 360° regeneration system from includes a range of various products that help the practitioner to select the right materials to achieve the optimum for their patient.
The botiss in-house development department has worked hard to develop a completely new product line for dentistry from a synthetic, absorbable class. A fully comprehensive GBR systemhas been created, consisting of a membrane and a fixation system. These products are based on new biodegradable metals – in this case absorbable magnesium in its metallic form. The idea behind the development of a new type of membranes was to get a product, which is strong but malleable and is easily absorbed by the body so that it does not need to be removed later. Information about the market release will follow.
In conclusion, botiss is constantly reviewing, adapting and complementing the 360° botiss regeneration system in order to provide you with biomaterials which are safe to use at any time.
Literature
1 Kampf et al. (2020). Persistence of coronaviruses on inanimate surfaces and their inactivation with biocidal agents. J Hosp Infect; 104(3):246-251.
2 Wen et al. (2019). Time Analysis of Alveolar Ridge Preservation Using a Combinations of Mineralized bone‐plug and dense – polytetrafluoroethylene membrane: A Histomorphometric Study. J Periodontol; 91(2):215-222.
3 Statement “SARS-CoV-2”, C+TBA 09.03.2020, available upon request
4 van Doremalen et al. (2020). Aerosol and surface stability of HCoV-19 (SARS-CoV-2) compared to SARS-CoV-1. N Engl J Med; 382:1564-1567
5 Zheng et al. (2020) Viral load dynamics and disease severity in patients infected with SARS-CoV-2 in Zhejiang province, China, January-March 2020: retrospective cohort study. BMJ (Clinical research ed.); 369 m1443.
6 Brown et al. (2000), New studies on the heat resistance of hamster-adapted scrapie agent: threshold survival after washing at 600 degrees C suggests an inorganic template of replication. PNAS; Vol. 97 No. 7, pp. 3418–3421.
7 Tadic and Epple. (2004), “A thorough physicochemical characterisation of 14 calcium phosphate-based bone substitution materials in comparison to natural bone”. Biomaterials; Vol. 25 No. 6, pp. 987–994.
8 Rothamel et al. Sinus floor elevation using a sintered, natural bone mineral. Zzi; 27(1) 2011.
9 Trajkovski et al. (2018). Hydrophilicity, Viscoelastic, and Physico chemical Properties Variations in Dental Bone Grafting Substitutes. Material; 11(2), 215.
10 Zafiropoulos et al. (2020). Open-Healing Socket Preservation with a Novel Dense Polytetrafluoroethylene (dPTFE) Membrane: A Retrospective Clinical Study. Medicina (Kaunas); 56(5):E216.
11 Radha R, Sreekanth D (2017). Insight of magnesium alloys and composites for orthopedic implant applications – a review. Journal of Magnesium and Alloys 5(3):286-312. Available at: https://www.sciencedirect.com/science/article/pii/S2213956717300415
12 Staiger MP, Pietak AM, Huadmai J, Dias G (2006). Magnesium and its alloys as orthopedic biomaterials: a review. Biomaterials. 2006 Mar;27(9):1728-34. Epub 2005 Oct 24.
13 Institute of Medicine (IOM) (1997). Dietary reference intakes for Calcium, Phosphorus, Magnesium, Vitamin D, and Fluoride. Food and Nutrition Board, Institute of Medicine. National Academy Press, Washington, D.C.
14 National Institute of Health (NIH) – Magnesium — Health Professional Fact Sheet website available at https://ods.od.nih.gov/factsheets/Magnesium-HealthProfessional/#en1. Accessed 14 May 2020.











